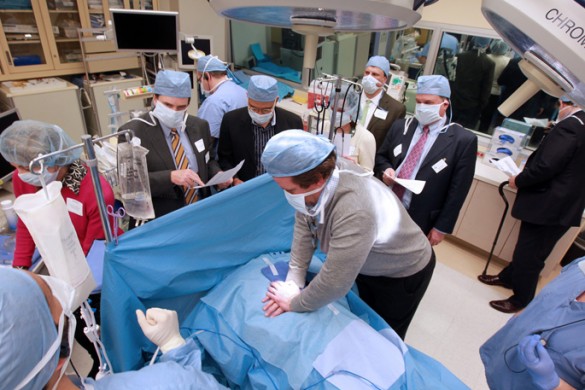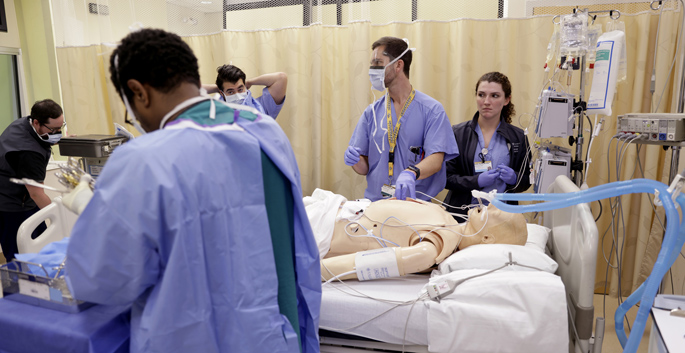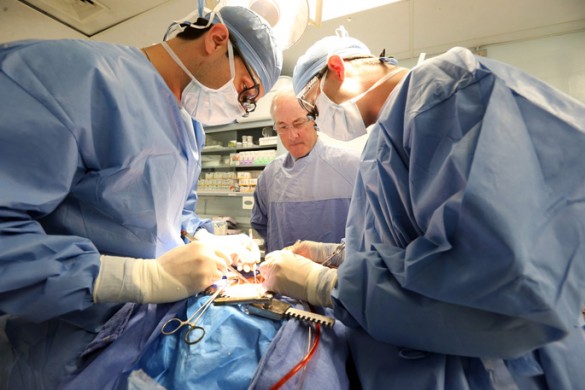
Just as pilots and members of the military go through boot camp and simulation exercises early in their training so they are prepared to respond in real-life situations, first-year cardiothoracic fellows at Vanderbilt University Medical Center (VUMC) recently experienced their own specially designed boot camp centered around a new high-fidelity simulator that realistically re-recreates cardiac procedures so they are better prepared for the operating room.
“The best time to train our fellows using simulation is at the beginning of their training, when they have the least knowledge and experience,” said Jonathan Nesbitt, M.D., director of the Cardiac Simulation Program. “By immediately imparting these skills early in training, we significantly compress the learning curve to allow them to work effectively and safely as fellows in the clinical realm.”
The month-long VUMC boot camp is the first of its kind in the country and was conducted in August over 42 consecutive four-hour sessions. The program was the culmination of nearly eight years of work, said Nesbitt, and its origin is in an eight-institution research study funded by the Agency for Healthcare Research and Quality (AHRQ) that investigated whether simulation training for cardiothoracic fellows can improve surgical skills and decision-making. Nesbitt was a co-principal investigator in the study.
A product of the AHRQ study was a 38-week cardiac surgery simulation curriculum which was modified and adapted for the VUMC boot camp.
The course covers basic components of cardiac surgery, cardiopulmonary bypass, coronary artery bypass grafting, aortic valve replacement, and catastrophic events that infrequently occur, such as massive air embolism and aortic dissection during bypass operations. Team training and communication are key components to each session.
For highly technical surgical specialties like cardiac surgery, surgical skills are acquired over many years of practice. When first learning those skills, cardiothoracic fellows are taught in an apprentice-style approach under the tutelage of the teaching faculty in the operating room.
Simulation training is another tool for teaching technical skills and occurs in a more controlled environment such as a laboratory.
Simulation training has been increasingly used in the surgical specialties because of changes in procedure types, along with the continued requisite of technical excellence.
“We are now able to recreate a cardiac operating room, in a simulated environment, because of a tool that we helped to develop, a device I call SimCAB,” said Nesbitt. “Because of SimCAB, our program was possible.”
SimCAB merges a heart-lung machine (HLM), a HLM simulator, and a real-tissue porcine heart model with artificial blood flow that is coupled to a pump that drives balloons inserted inside the heart to create a beating heart.
The SimCAB hardware is driven by a computer software package and can be modified for limitless operating room scenarios. Changes in vital signs are continuously monitored, allowing the fellows to practice management skills in a controlled environment while also honing technical skills during a simulated operation.
“This is a very sophisticated model with programmed interactions between three components to create a very realistic cause and effect relationship,” said Perfusion Program Director Nicole Michaud, who worked with Nesbitt to develop SimCAB and the boot camp curriculum.
“In order to create the highest realism, we have an actual tissue model and surgical arena that mimics the operating room, including the personnel and equipment. The tissue model, beating in synchrony with the hemodynamics, creates the ultimate learning environment. For example, when the perfusionist initiates controlled cardiac arrest in the operating room, the heart starts to slow down, then stops; the tissue model in our simulation sessions does the same thing.”
In addition to fellows, the simulation sessions include a perfusionist who runs the heart-lung machine, a surgical tech who hands instruments and sutures to the fellows, and anesthesiology team members. One goal of the sessions is for the group to learn and reinforce the skills that make a team successful, especially during an event that is far from routine, said Michaud.
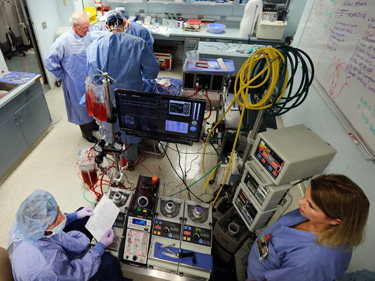
“During the first three weeks of doing this, the fellows’ abilities skyrocketed,” said Nesbitt as he oversaw the inaugural boot camp.
“It really was amazing to watch their progress and their increased comfort level. In the future, if something goes wrong in the main operating room, they’re now equipped to better handle the problem in a composed, organized fashion. They can fall back on what they’ve learned in the simulation lab.”
John Evans, M.D., who completed his general surgery residency at University of Alabama before coming to Vanderbilt, said he felt like the month-long immersive simulation training has better prepared him for the operating room.
“I feel a lot more comfortable about cardiopulmonary bypass and many other aspects of cardiac cases as a result of this simulation training,” Evans said. “And this intensive exposure over several weeks, as opposed to several months of trying to figure it out slowly, has been invaluable. When you have time dedicated to an uninterrupted simulation experience, that’s when you really benefit.”
Michael Archer, D.O, who completed his general surgery residency at Alleghany General Hospital, said his previous simulation training had only been on static models, so using a dynamic model to improve his cardiac surgery skills was a welcome change.
“When I heard about this month-long simulation training, I was excited about it, but I was also a little worried about being away from the operating room for that long,” Archer said.
“But when we come into the simulation lab, we’re focused. It’s very intense. When we go home, we’re physically exhausted. It’s just like going into the operating room every day.”
Nesbitt credits the support and commitment of the Cardiac Surgery faculty and the surgical laboratory staff for the boot camp’s success. Countless hours of preparation, teaching and proctoring occurred throughout the month, he said.
“In addition, the faculty’s participation at an extremely high level allowed the fellows and the attending physicians to develop a bit of camaraderie prior to entering the real-time setting of the operating room.
“Our residents have benefited significantly. They are now better equipped to enter their clinical training with confidence, with a higher level of skill, and with an enhanced ability to practice their art more safely,” Nesbitt said.