BY KATHY WHITNEY
HEART PHOTO BY ROBERT CLARK / INSTITUTE
A 53-year-old patient arrives at Vanderbilt University Hospital early one morning for a procedure to open up a blockage in his left anterior descending artery by placing a single stent to his heart via the radial artery in his wrist. That same evening he returns to his home in Fort Campbell, Ky.
Inside the Monroe Carell Jr. Children’s Hospital at Vanderbilt, a young couple envisions a real future for their 2-month-old son, who was born with an enlarged heart and spent the first seven weeks of his life on extracorporeal membrane oxygenation (ECMO) before receiving a heart transplant.
“He will go to school, play sports, do normal little boy things,” says his mom.
Across campus, in a laboratory in the Robinson Research Building, investigators use fluorescence microscopy to screen chemical compounds for their effects on heart size in developing zebrafish embryos. Their findings eventually could lead to new approaches for cardiac regeneration and repair in humans.
A few miles away, in a light-filled suite of Vanderbilt offices that once were part of a dying 100 Oaks shopping mall, a middle-aged patient and her cardiologist discuss her options for using statin drugs to treat high cholesterol. Genetic screening will help determine which drugs are most likely to work for her and which will have the fewest side effects.
Forty miles down Interstate 65 in Columbia, Tenn., Dr. Rebecca Hung, assistant professor of clinical medicine, collaborates with cardiologists at Vanderbilt Heart-Columbia and Maury Regional Medical Center to bring advanced heart care to patients who are too sick to make the drive to Nashville. The Columbia facility is part of the vast Vanderbilt Heart network, dotting not only the state of Tennessee but parts of Kentucky, with 23 heart clinic locations from Johnson City to Waynesboro.
Depending on your perspective, the business of mending broken hearts at Vanderbilt is either very good or very bad.
No. 1 with a Bullet
“Cardiovascular disease is the leading cause of death in the United States—more than all forms of cancer combined,” says Dr. Keith Churchwell, executive director and chief medical officer for the Vanderbilt Heart and Vascular Institute. “If you take all other diseases, they don’t equal heart disease. It’s No. 1 with a bullet.”
More than 60 million Americans are living with cardiovascular disease, and the costs associated with it added up to an estimated $500 billion in 2012 alone. One-third of deaths in this country are due to cardiovascular disease—and Tennessee is ranked third in annual death rate from heart attack and stroke.
During the past decade Vanderbilt has poured tremendous effort into heart care, making it the region’s leading heart care provider. VUMC is the first U.S. medical center to give a drug called GGF2 to patients recovering from heart failure. In trials the drug has helped regrow damaged heart muscle.

“We have entered another renaissance in cardiovascular technology and how it enables us to care for patients,” says Churchwell. “In the late 1970s we witnessed a new age of revascularization with angioplasty. Now we are looking at the age in which diagnostic and therapeutic techniques are taking another significant leap forward. As an example, cardiologists and cardiac surgeons can now replace an aortic valve without opening the sternum—a tremendous advance which will usher in other technological advances and new care models that should be more efficient, less costly, and better for patients.”
At the forefront of Vanderbilt’s work is the PREDICT (Pharmacogenomic Resource for Enhanced Decisions in Care and Treatment) program, the first of its kind in a U.S. academic medical center to embed genetic information of patients using statin drugs into their electronic medical records. More than 9,000 patients to date have benefited from Vanderbilt’s PREDICT program.
“PREDICT began with the antiplatelet drug clopidogrel [Plavix] and the cholesterol-lowering drug simvastatin [Zocor], and will be expanded soon to include a host of other drugs,” says Dr. Jeff Balser, MD’90, PhD’90, vice chancellor for health affairs and dean of the School of Medicine. “We are the very first medical center to do this in a way that scales across the health system and which is accessible to patients.”
Although most people respond in the same way to a given drug, there are always individuals who experience harmful side effects or don’t respond to the treatment.
“You can think of it this way: If you take 10 different drugs, you will probably react normally to nine of them, but your reaction to the 10th will be abnormal,” says Dr. Dan Roden, assistant vice chancellor for personalized medicine. “We just wish we knew which one that will be.”
Scientists are convinced that most of this variability is due to differences in individual genomes. Vanderbilt is pushing forward the frontiers of personalized medicine through its massive DNA databank, called BioVU, and through PREDICT, which helps physicians choose the best medications for their patients.
PREDICT is a clinical decision-support program that tests Vanderbilt patients for genetic variations that affect how the body responds to commonly prescribed drugs. That information is shared with their physicians to help them choose the drugs most likely to work for their patients and least likely to cause serious side effects.
In 2011, Vanderbilt doctors began screening patients who take commonly prescribed statin drugs for a rare genetic variation that can increase risks for side effects. Statin drugs, among the world’s most commonly prescribed medications, are used to lower cholesterol levels in the blood. One in four Americans ages 45 and older is taking a statin drug.
Simvastatin, the generic form of the statin Zocor, is one of the most widely prescribed drugs in the United States and is effective in reducing LDL-cholesterol levels and lowering the risk for heart attacks and strokes. But growing evidence indicates that about 2 percent of patients taking 80 milligrams of simvastatin per day will experience muscle aches that could lead to muscle damage. In extreme cases complications can be more severe, such as kidney damage and even death.
The risk for developing complications is increased when a patient carries even a single genetic variation, notes Roden. “If you have two copies of the SLC01B1 gene, you’re at an almost 20-fold increased risk of muscle toxicity,” he says.
“We’re just reducing the odds. That’s what applying genetics at the bedside is all about. It expands what you know about the individual patient.”
Finding the Right Statin
When O.T. Haynes of Lebanon, Tenn., first starting seeing Vanderbilt cardiologist Dr. David Hansen for treatment of coronary artery disease, it was hard to predict which statin would help control the 67-year-old man’s high cholesterol. Hansen prescribed several for Haynes, trying to find one that achieved his cholesterol goal without causing debilitating side effects.
“A full house of drugs was tried on him: simvastatin, atorvastatin, fluva-statin and rosuvastatin,” says Hansen, associate professor of medicine. “Each time he reported back that his muscles started aching and he felt weak.”
Haynes had to stop those medications. If one is not careful about stopping when symptoms occur, the drug can lead to a breakdown of skeletal muscle and the release of cellular components from muscle that travel to kidneys and cause acute renal failure.
Then the PREDICT test became available.
“I ordered testing for him, and it turns out Mr. Haynes received one defective copy of the SLC01B1 gene from his parents, and the other gene is what we’d call normal,” Hansen says. “That puts people at intermediate myopathy risk for having side effects from simvastatin.”
Haynes was switched to lovastatin, which has not produced the same adverse effects. His LDL level has reached its target goal.
“This patient had a lot of trial and error over a four-year period prior to the availability of the PREDICT test,” Hansen says. “When it first came out, I started using it. As a practicing cardiologist, a very good percentage of my patients have had the PREDICT test. It expands what I know about each of my patients.”
Simvastatin and most other statins use the same metabolic pathway as a way of being broken down into smaller bits and being excreted from the body. Based on this information, Vanderbilt was able to publish the first international gene-based dosing guideline for statins earlier this year.
“The clinical community has been waiting for this type of guidance for several years,” says Dr. Russ Wilke, director of genomics and cardiovascular risk at Vanderbilt and lead author of the guideline.
Heart Failure: A Multipronged Approach
Statins may be effective in treating many cases of high cholesterol, but heart failure remains the leading cause of hospital admissions and subsequent death in the United States. It occurs when the heart cannot pump enough blood to the body’s organs, depriving the body of needed oxygen and nutrients. Coronary artery disease is just one of several conditions that can lead to heart failure. Others include complex valvular disease, cardiomyopathy and myocardial infarction.
The Vanderbilt Heart and Vascular Institute treats patients with heart failure using multidisciplinary teams that may include cardiac and transplant surgeons, specially trained and certified cardiologists, nurse practitioners, social workers, dieticians, psychologists, pharmacists and infectious disease specialists.
Vanderbilt’s transplant surgeons have performed more than 550 heart transplants since the first procedure was done at VUMC in 1985. Vanderbilt performed Tennessee’s first pediatric transplant, first heart-lung transplant, and first single lung transplant. VUMC also had the first program in Tennessee to perform heart transplants in infants with hypoplastic left heart syndrome.
In addition, Vanderbilt was the seventh center in the nation and first in the Southeast to successfully implant the second-generation electrical left ventricular assist device (Novacor LVAD) as a bridge to transplantation. The use of this device and other similar devices is now standard practice for bridge-to-transplantation in severely unstable patients who are awaiting suitable organs.
For some patients open-heart surgery poses too great a risk. Nearly 200,000 people each year are diagnosed with aortic stenosis, a narrowing of the main valve allowing blood to leave the heart. Seventy-five percent of those diagnosed are deemed high-risk or ineligible for open-heart surgery—the standard therapy.
In 2011 the Vanderbilt Heart and Vascular Institute embarked on a clinical trial using artificial valves to replace a patient’s defective one without opening the chest, and has since performed more than 100 transcatheter aortic heart valve-replacement (TAVR) procedures. Vanderbilt is one of a few medical centers in the country to offer both the CoreValve and the Edwards SAPIEN valve.
“There are no other options for this group of patients,” says Dr. David Zhao, director of the Cardiovascular Catheterization Lab and Interventional Cardiology.
Using transcatheter aortic valve implantation, the artificial valve is attached to a wire frame and guided by catheter through the groin to the heart. Once inserted inside the defective valve, the wire frame expands, allowing the new aortic valve to open and immediately begin to pump blood.
Compared to the four to six hours typical in open-heart surgeries, this procedure calls for a smaller incision and takes about 90 minutes to complete.
“We have clearly established Vanderbilt as a leader in this minimally invasive procedure for valve replacement,” says Dr. John Byrne, William S. Stoney Professor and chair of the Department of Cardiac Surgery. He predicts the nonsurgical valve-replacement technique will become a standard therapy in the next three to five years.
“Medical technology does not stand still,” says Churchwell. “It is always evolving and developing new ways to image and evaluate the body to obtain precise and extremely accurate evaluation of disease processes. How to keep up without breaking the bank continues to be a tremendous challenge. New medications, new technology and better education are our greatest opportunities to impact heart health.”
It took all of that and more when Anthony Nolan arrived at Vanderbilt last summer.
When Collaboration Is Crucial
Stacey Browning, a Cardiovascular Intensive Care Unit charge nurse, remembers getting a report last July about a heart attack patient who was being transported to her unit from an outside hospital and thinking her unit was receiving a patient who would not recover.
“We’re going to have to tell the family when they get here that we’re sorry, but there is nothing we can do, because that’s how bad it sounded,” she recalls.
The patient was Anthony Nolan, a former member of the U.S. military, a recipient of the Bronze Star and a professional skydiver. The 43-year-old father of two was the picture of health until his heart suddenly stopped working while he was watching television with his wife, Leila.
Leila performed CPR while they waited for an ambulance to arrive at their house in Hermitage, Tenn. From there Nolan was taken to an area hospital where 100 percent blockage in two coronary arteries was discovered. Doctors inserted a balloon pump to perfuse the arteries, stabilized him, and transported him to another facility where he underwent quintuple coronary artery bypass surgery.
He became unstable and was taken back to the cath lab, where an Impella left ventricular assist device (VAD) was implanted. Shortly after, his heart went into recurrent ventricular fibrillation and he was “shocked” back to life more than 60 times with a defibrillator.
Four days after his bypass surgery, he was transferred to Vanderbilt to consider further mechanical circulatory support. He was taken to the operating room to be placed on ECMO, where the blood is circulated through an artificial heart and lung. Continuous dialysis was begun when Nolan began to experience kidney failure.
Five days later his surgical team, led by Dr. Simon Maltais, took him off ECMO and implanted bilateral CentriMag ventricular assist devices, which supported both sides of his heart to allow it to recover from the acute myocardial infarction.
Nolan was in and out of consciousness for several days, during which time he was evaluated for heart transplantation. During a two-week period, the Vanderbilt team weaned him from VAD support and determined his heart had recovered completely. The CentriMag VADS were removed and transitioned to an intra-aortic balloon pump.
All told, he had six procedures and was kept alive with four different devices.
“I have never seen a case like this,” Maltais says. “He was so ill when he arrived at Vanderbilt. It took a tremendous amount of collaboration among cardiologists, cardiac surgeons, and the expertise of the ICU staff to take care of him and move him forward on these devices to allow him to recover.”
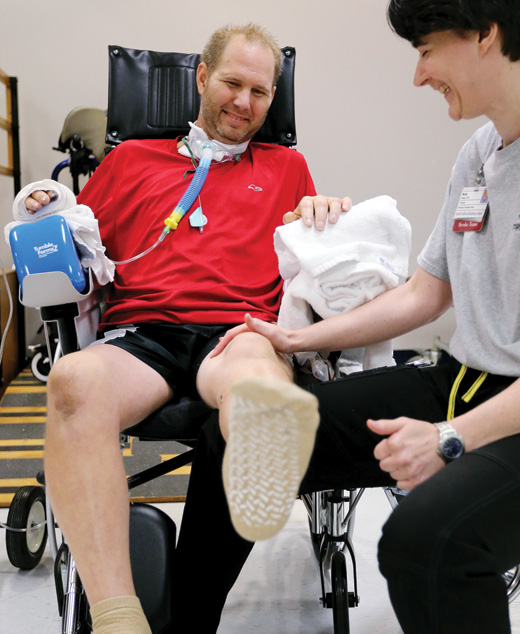
Now, after a stay at Vanderbilt Stallworth Rehabilitation Hospital, Nolan is enjoying life back at home with his wife and twin 3-year-old daughters. He doesn’t remember much of his hospital time, but smiles as he listens to his wife and nurse retell the story.
“I got beaten up pretty bad,” he says. “It feels awesome [to hear the story] because I’m sitting here listening to it.”
In fact, Nolan has improved to the point that he will not need a heart transplant. For a man who was given a 5 percent chance of survival when he arrived at Vanderbilt, his words are music to his nurses’ ears.
“In the five years I’ve worked here on this unit, I can’t recall another patient who has gone through four devices. He is amazing,” Browning says.
“Do One Little Thing”
As options for keeping patients alive and healthy proliferate, of course, so do the costs of care. That’s just one reason why the most important member of a cardiac care team is the patient himself. Having access to medical information is only one part of personalized medicine.
Prevention, says Churchwell, could help reduce cardiovascular disease by a whopping 80 percent—and most of it is within the patient’s grasp.
“We have come to terms with the knowledge that we must better educate our patients about their medical problems to have greater success with their long-term treatment,” Churchwell says. “We primarily offer short-term solutions to lifelong problems. We have to arm our patients with better tools—medicines, technology and understanding—so they can meet the challenges of cardiovascular disease with greater lifelong success.
“Getting active is one of the very best behaviors that can save our lives. If you’re not doing anything, do one little thing. If you’re doing something, do a little more. Little steps add up to a big impact.
“Eat more fresh fruits and vegetables,” he adds. “Stop smoking. Bake or grill—don’t fry. Lower your sodium and sugar intake. Lose a few pounds. Check your blood pressure, cholesterol and glucose.
“That would make my services much less in demand. I pray for that day to come.”