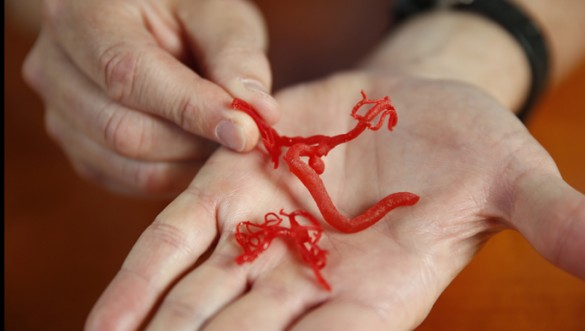
A brain aneurysm is often likened to a ticking time bomb — the bulge in a blood vessel is just waiting to burst, with devastating consequences for motor and cognitive function.
To help patients cope, give them more information about the disease process and let them network with other patients, Vanderbilt University Medical Center holds a monthly Brain Aneurysm Support Group.
Started in 2011, patients, family and friends and medical staff gather the first Thursday of each month to listen to a featured speaker, have a question and answer session and share their tips and stories with each other.
“There are only about 30,000 or so ruptured aneurysms in the United States per year. So from a population standpoint, that’s not a huge percentage. Patients are very isolated when they go home because they don’t know anybody else around them who has gone through it,” said Kiersten Espaillat, APRN, R.N., stroke services coordinator, who helps facilitate the support group along with nurses Marianne Rickel, R.N., and LaSheryl Brown, LPN.
At a support group meeting, speakers will discuss the basics of aneurysm, research being conducted, what to expect during recovery and how to deal with issues like mobility, memory loss or depression.
Presentations are limited to 20 minutes because organizers found that the participants benefitted most from talking with each other.
“Someone says something and you see the others nodding and understanding. They have great ideas to share. Someone will say they are tired and fatigued and someone will give advice on what they did,” Rickel said.
For Martha Matthews, who survived a ruptured aneurysm 10 years ago at age 57, that community aspect is what keeps her coming back month after month. But it was intimidating at first, as she met fellow patients and saw the effects of the disease.
“I was so discouraged when I saw some of the people. But my sister said I had to keep coming. She said when people saw me they would have hope,” Matthews recalled.
After treatment at Vanderbilt and rehab at Stallworth Rehabilitation Hospital, Matthews is back to running her catering business and living what she calls her “new normal.”
“I had to learn to walk, talk and think again. I made lots of progress the first two years and it’s more gradual now. I don’t think as clearly or quickly, but I just keep pushing and keep myself busy.”
Patients who experience a ruptured aneurysm often present at a hospital with a severe headache. An eerily common refrain is that they’re experiencing the worst headache of their life.
The majority of brain aneurysms form at the base of the brain because there is a lot of blood flow and many branching blood vessels. As blood constantly pounds against that branch point, a bubble can form and eventually rupture. Then it is a race against the clock to prevent further bleeding and restore proper blood flow to brain tissue to preserve function.
Other patients may have a brain scan for an unrelated problem — chronic sinus congestion or a head injury — and inadvertently discover an aneurysm. The question then becomes when and how to treat.
“Modern imaging technology has completely changed the game. It gives us the ability to look at the aneurysm in incredible detail and personalize their care for the very best treatment,” said J Mocco, M.D., M.S., associate professor of Neurological Surgery, who specializes in the treatment of ruptured and unruptured aneurysms, as well as other types of stroke.
At Vanderbilt, surgeons can evaluate the “flow dynamics” of an aneurysm, showing how blood moves through the bulge and estimating where its weak points may be. There are also three-dimensional angiograms that let surgeons visualize the aneurysm and nearby blood vessels in a 3-D environment.
Neurosurgeons at Vanderbilt follow the ISUIA (International Study of Unruptured Intracranial Aneurysms) guidelines, which evaluate the risk of an aneurysm and provide guidelines for prophylactic treatment. Mocco is one of the current leaders of the ISUIA trial.
Although 7 mm is the general threshold size to treat an aneurysm, Mocco also considers age, location, relation to other critical structures and the shape of an aneurysm.
Gary Gress’ aneurysm measured 8 mm x10 mm, a definite for treatment under ISUIA guidelines. In 2010 at age 67, his doctor ordered a CT scan to investigate a sinus problem. A constant comedian, Gress joked about the space she would find in his head. But when she had to break the news of the aneurysm, he was all seriousness.
“It was no surprise to me; I had high blood pressure and high cholesterol and was a smoker,” he said. “She said I had to go to Vanderbilt because she didn’t know if it was bleeding or not.”
Luckily it wasn’t, and Gress opted for treatment with endovascular embolization. Through an incision in the leg, platinum coils are threaded through the blood vessels into the aneurysm, essentially packing the bubble with metal so blood can no longer enter. It’s a less-invasive alternative to clipping the aneurysm through open surgery.
Gress started coming to the support group three months ago and has a steady supply of jokes for attendees.
“My wife says all I do is tell jokes, but I say why be serious? There’s nothing I can do about this.”
Rickel said it is rewarding to see the group gather each month to share advice and celebrate recoveries.
“We had one lady who came who had ruptured. She was on a walker and always had someone there to help her. Then later she was driving herself and living alone. It was wonderful to see that improvement every month,” she said.
For more information about the Brain Aneurysm Support Group, visit www.bafound.org/node/466 or contact kiersten.brown@vanderbilt.edu or 936-3157.












